Social security has worked well for 89 years in the exact way it was set up and how it was promised. In the modern age, that is more than the average lifetime.Of course it’s a dig at the institution which has never worked the way it was sold or promised, which is going to be insolvent if it isn’t fixed, and which can’t be fixed because it is a political third rail.
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
American Healthcare continues to go backward
- Thread starter steross
- Start date
The very first recipient put in $24 and received over $22,000 for a 92,000% return.Social security has worked well for 89 years in the exact way it was set up and how it was promised. In the modern age, that is more than the average lifetime.
Anecdotal reply that is not responsive to the proposition advanced.The very first recipient put in $24 and received over $22,000 for a 92,000% return.
Polds4OSU
Marshall
she also only worked for 2 years and 10 months when social security was being collected. Most of here career there was NO such thing as social securityThe very first recipient put in $24 and received over $22,000 for a 92,000% .
So she only paid into social security for ~34 months from 1937 to 1939
Then retired and on Jan 31st 1940 Drew her first Social Security Payout check at the Age of 65.
She then died 35 YEARS later at the Age of 100 in 1975 having paid into Social Security for less than 3 years and drawing payments from it for 35 YEARS.
She was paid an Avg of $654 PER YEAR from Social Security from 1940 till 1975
(In today's money that would be an avg payout of $14,700 per year over 35 years)
Which is more important, the n=1 example you keep bringing up or the n=100's of millions (~78 million americans are getting SS checks this year)?The very first recipient put in $24 and received over $22,000 for a 92,000% return.
They are an exception and you know better than to do this with your background and knowledge of statistics.
The problems are:Which is more important, the n=1 example you keep bringing up or the n=100's of millions (~78 million americans are getting SS checks this year)?
They are an exception and you know better than to do this with your background and knowledge of statistics.
Most people outlive their contributions. Ida Mae Fuller is the rule, not the exception.
We don’t have enough new payers to keep it solvent.
We can’t fix it because it is a political third rail.
Trump: "We'll be announcing something very soon on pharmaceuticals. We're gonna give people about a year, year and a half to come in, and after that they're gonna be tariffed if they have to bring the pharmaceuticals into the country at a very high rate, like 200 percent."

Oh lord…Trump: "We'll be announcing something very soon on pharmaceuticals. We're gonna give people about a year, year and a half to come in, and after that they're gonna be tariffed if they have to bring the pharmaceuticals into the country at a very high rate, like 200 percent."
I’ve been saying for years and years and years that we subsidize the rest of the world by paying higher prices for prescription medications here in the US and it seemed for a minute that someone in Washington had figured it out and might do something about it… but… when you have a hammer, everything looks like a nail.
View attachment 12653
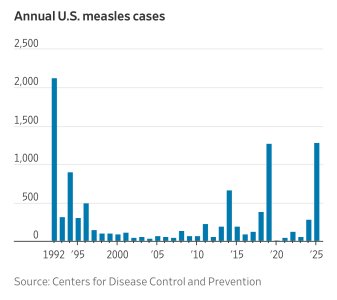
Measles cases at a three decade high, almost all cases unvaxxed or unknown vax status.
What happened in the early 90's?
Polds4OSU
Marshall
What happened in the early 90's?
How Public Health Outreach Ended A 1990s Measles Outbreak And What's Different Now
The outbreak from 1989 through 1991 was much larger than today's, with more than 27,000 cases in 1990 alone. But the conditions that lead to that outbreak and what it took to end it are dramatically different from the ones the U.S. is seeing today.The bulk of cases today are concentrated in New York state. As of Monday, New York City alone reports 498 cases, with 34 people hospitalized, since the outbreak began last September.
In New York state, public health authorities attribute the outbreak to anti-vaccination sentiments among a small subgroup of religious Orthodox Jewish residents among whom the virus has spread. The outbreak in the early 1990s hit poor black and Latino communities the hardest, in Central Brooklyn, upper Manhattan and the South Bronx.
The outbreak in New York City took off in the spring of 1990. And once the public health response got underway, parents got on board.
"Children were dying," says Dr. Irwin Redlener, who founded the Children's Health Fund to bring health care to New York City's poorest areas. "It was like all hands on deck. The city, the not-for-profit organizations, were all focused on the same mission with the enthusiasm of parents."
According to news reports from the time, criminal courts had to halt proceedings when inmates at the Rikers Island jail got sick. There were outbreaks on college campuses and in homeless shelters. One defunct hotel turned city shelter that Redlener visited was so overcrowded that it was an outbreak waiting to happen, he says.
"The conditions in the hotel and the lack of access to care — you have basically set up a scenario that is very conducive to the spread of a disease like measles," says Redlener.
The outbreak continued that fall, into the next year and through the summer of 1991. By the time it was over, there were more than 5,000 measles cases in the city and at least 21 deaths. It wasn't just in New York City either; starting in 1989, Chicago, Los Angeles, Houston and Philadelphia were experiencing large outbreaks as well. From 1989 through 1991, more than 55,000 were sickened and more than 100 people died across the United States, the highest numbers since the early 1970s, according to data from the CDC.
Public health historians partially attribute the outbreak to budget cuts during President Ronald Reagan's administration that affected federal funds directed toward immunization and public health initiatives.
"There was just less White House support for childhood immunization," says Elena Conis, an associate professor at the University of California, Berkeley, where she specializes in medical history.
Immunization rates peaked in the early 1980s because of investment during the prior administration of President Jimmy Carter. There was just one death attributed to measles in 1984, the lowest number ever recorded by the CDC. But as federal investment didn't keep up with inflation or with increases in the cost of the vaccine, immunization levels crept downward, particularly in areas where parents couldn't afford vaccinations.
Some federal funds that had been earmarked for immunizations in the past were instead given in lump sums to states, Conis says. And according to Conis, there was a third issue.
"We had a health care system that simply wasn't designed to serve low-income kids living in cities who were more reliant on public clinics, which weren't necessarily open all the time ... or were few and far between," Conis says.
By the time the outbreak hit in 1990, the CDC estimated that about half of all inner-city toddlers in New York City had not been vaccinated by their second birthday.
"Over the past years of tight budgets, the immunization programs have been eroded. ... The results have been predictable," Rep. Henry Waxman of California said at a 1991 hearing about the nationwide outbreaks. "The problem is clear to see. Vaccination programs are limited. Clinics are inaccessible. Appointments are required, and waiting lists have also grown."
Even worse, without access to preventive care, kids who got really sick with measles ended up in the hospital.
"We saw ... a lot of kids with measles and pneumonia, measles and croup, measles and acute encephalitis," says Dr. Joel Forman, who was just starting his pediatric residency at Mount Sinai Hospital in New York City in the summer 1990. Years later, one of Forman's patients died from an extremely rare complication from measles called subacute sclerosing panencephalitis.
"When he first was sick of measles, he was 7 months — I remember that," Forman says. "He recovered uneventfully and only presented years later with a lethal complication."
By the summer of 1991, New York officials redoubled their efforts, with Mayor David Dinkins and Gov. Mario Cuomo working in concert. Measles messages were flashed across the giant Sony computer screen in Times Square. Buses outfitted as mobile health clinics offered free immunizations. One immunization drive featured Michelangelo from the Teenage Mutant Ninja Turtles, who emerged from a sewer at the South Street Seaport to encourage kids to get the vaccine. Shots were given to kids at parks, beaches and outdoor concerts, including one featuring Latin jazz icon Tito Puente. The outbreak eventually petered out.
On the federal level, things were changing too. In 1993, newly elected President Bill Clinton pledged to raise childhood immunization rates. That year, Congress created the Vaccines for Children program, which funded vaccinations for children whose parents couldn't afford them, and federal funding increased sevenfold from $37 million in 1990 to $261 million in 1995.
Measles vaccination rates climbed above 90%, where they've remained in most places. New York became the first state to require a measles booster shot, which is now required across the country and is said by the CDC to increase the effectiveness of the vaccine from 93% to 97%.
Today's measles outbreak in New York is far smaller than the one in the 1990s. And the reasons behind it are very different.
"Then, it was people who couldn't get access to health care," Redlener says. "Now it's this cultlike atmosphere of people who are refusing to immunize."
Since last fall when the outbreak began, city health officials say, more than 20,000 doses of the measles, mumps and rubella vaccine have been administered to children in Brooklyn neighborhoods. City health officials have met with community leaders, published ads in community papers, sent out robocalls and hosted conference calls with doctors.
Still, they're facing a small but mobilized subgroup of the ultra-Orthodox community that opposes vaccines and has links to the larger, secular anti-vaccination movement. This has hindered the city's ability to stop the spread of measles so far, said Dr. Demetre Daskalakis, deputy health commissioner, at an April 17 meeting of the city's Board of Health.
He spoke of parents not seeking medical care for sick kids or intentionally exposing children to the measles virus at "measles parties," and of the spread of misinformation about the vaccine.
"There's a lot of things we're working against," he said
In response to the measles outbreaks…
1996: The American Pharmacists Association (APhA) created a training program for pharmacists to administer vaccines.
1996–2000s: State laws began changing to allow pharmacists to vaccinate. It started with flu shots and gradually expanded to others like shingles, pneumonia, and later COVID-19.
2010s: Most states had authorized pharmacists to give a wide range of vaccines.
Pharmacists are currently authorized to vaccinate in all 50 states.
1996: The American Pharmacists Association (APhA) created a training program for pharmacists to administer vaccines.
1996–2000s: State laws began changing to allow pharmacists to vaccinate. It started with flu shots and gradually expanded to others like shingles, pneumonia, and later COVID-19.
2010s: Most states had authorized pharmacists to give a wide range of vaccines.
Pharmacists are currently authorized to vaccinate in all 50 states.
Polds4OSU
Marshall
Fox Host: One problem, Trump is suggesting we may have 200% tariffs on pharmaceuticals. It's going to take a long time for domestic pharmaceutical production to replace that. What do you do in the interim? How will that 200% tariff interfere with the ability to get pharmaceuticals that cannot be made sufficiently now domestically?
Trump advisor: Well, it'll create the incentives for industry to accelerate the timeline...
Fox Host: Right. But what about now? That's the problem

 www.threads.com
www.threads.com
Trump advisor: Well, it'll create the incentives for industry to accelerate the timeline...
Fox Host: Right. But what about now? That's the problem

FactPost (@factpostnews) on Threads
Fox Host: One problem, Trump is suggesting we may have 200% tariffs on pharmaceuticals. It's going to take a long time for domestic pharmaceutical production to replace that. What do you do in the interim? How will that 200% tariff interfere with the ability to get pharmaceuticals that cannot be...
 www.threads.com
www.threads.com
When we built a school of pharmacy in Ohio, one of the essential pieces was a dispensing lab where we teach students how to do traditional pharmacist things such as sterile and non-sterile compounding. We had a consultant, a friend of the dean's, who wanted us to make our sterile compounding lab a class A clean room where we could do large quantity sterile compounding after hours, essentially make the lab dual use, teaching during the day, compounding at night. I had managed, for a brief period early in my career, a home health care pharmacy with a sterile compounding lab. This was before class A and USP 797 were required, but still, the setup and maintenance was expensive. The dean had never done this kind of work. As we got into the plans, the difference between making the sterile compounding lab a mock sterile compounding lab and a class A environment was... about a half million. One room.Fox Host: One problem, Trump is suggesting we may have 200% tariffs on pharmaceuticals. It's going to take a long time for domestic pharmaceutical production to replace that. What do you do in the interim? How will that 200% tariff interfere with the ability to get pharmaceuticals that cannot be made sufficiently now domestically?
Trump advisor: Well, it'll create the incentives for industry to accelerate the timeline...
Fox Host: Right. But what about now? That's the problem

FactPost (@factpostnews) on Threads
Fox Host: One problem, Trump is suggesting we may have 200% tariffs on pharmaceuticals. It's going to take a long time for domestic pharmaceutical production to replace that. What do you do in the interim? How will that 200% tariff interfere with the ability to get pharmaceuticals that cannot be...www.threads.com
Now scale that up for a pharmaceutical company that produces generic medications and now needs to move their operations from China or India to the US. To replace the generics that come from China and India we are talking hundreds of billions in investment.
To put it simply, it can't be done. "We'll create incentives". It's like when Kip Chalmers ordered the Taggart Comet to moved forward in the tunnel using the coal burning engine, which then killed everyone onboard.
Polds4OSU
Marshall
Ok....so the Sec of Homeland Security is Also running FEMA and now she gets to determine THIS !!??
Secretary Kristi Noem claimed that she and RFK Jr. will be deciding what research on viruses can be conducted at NIH during a recent hearing in the United States Senate.
'It Must Be Correct Research': Sec. Kristi Noem Says She Will Be The Arbiter Of Disease Research At NIH During Senate Testimony
Secretary Kristi Noem claimed that she and RFK Jr. will be deciding what research on viruses can be conducted at NIH during a recent hearing in the United States Senate.
Ok....so the Sec of Homeland Security is Also running FEMA and now she gets to determine THIS !!??
'It Must Be Correct Research': Sec. Kristi Noem Says She Will Be The Arbiter Of Disease Research At NIH During Senate Testimony
Secretary Kristi Noem claimed that she and RFK Jr. will be deciding what research on viruses can be conducted at NIH during a recent hearing in the United States Senate.
Its like he only trusts a handful of people. And not because they are that talented, but because they are a bunch of yes men who won't cross him.
If this is the way he runs his business no wonder hes had a bunch of bankruptcies
She wouldn’t know correct research if it bit her in the a**, and I’m willing to volunteer to test my theory.Ok....so the Sec of Homeland Security is Also running FEMA and now she gets to determine THIS !!??
'It Must Be Correct Research': Sec. Kristi Noem Says She Will Be The Arbiter Of Disease Research At NIH During Senate Testimony
Secretary Kristi Noem claimed that she and RFK Jr. will be deciding what research on viruses can be conducted at NIH during a recent hearing in the United States Senate.
I've been under the impression that his admin qualifications are:Its like he only trusts a handful of people. And not because they are that talented, but because they are a bunch of yes men who won't cross him.
If this is the way he runs his business no wonder hes had a bunch of bankruptcies
Men-Are they blindly loyal?
Women-Must be hot
Similar threads
- Replies
- 48
- Views
- 2K
- Replies
- 1
- Views
- 409
- Replies
- 0
- Views
- 362